
As we drove out of Belfast for the last time six months ago, we passed under a sculpture of a sphere within a sphere. Two geodesic wire creations, one nestled within the other. The guys had gotten waylaid on their way to park the car as we checked into our hotel and this was a landmark that they recognized. I couldn’t help but think what that visionary, designer of the geodesic dome, Buckminster Fuller would have thought. His words are the title of this post. Smart man, B.
That the sculpture, named RISE, represents a new chapter and seems to be apropos today as well.
When Rich first went through chemo in 2004, he was advised by an oncology nurse to keep moving… whatever he could do, keep moving. She went on to explain that he would feel better and could help with side effects.
As always, Rich took this to heart and, once he wasn’t able to work any longer, he walked. He walked the trails at our nearby park as the neuropathy took hold and he couldn’t feel his feet. He kept walking those paths until the numbness was up to his knees. He said, “It’s not very busy at the park when I go. If I fell, I don’t know how I could get help!” So, he began walking our neighborhood instead. When that got to be too tough, he walked our small garden. He walked laps throughout the house. He kept walking.
When we began our journey again ten years later, he walked. He walked from the train to the office. When again he had to stop working, he continued his walks at home. Whenever in the hospital, we walked the halls. The nurse had said to keep moving and move he did.
When we entered the stem cell isolation unit, he walked, counting his laps and trying to improve each day. For four weeks we strolled up and down the hallway within a hallway, marking our pace and distance. In all that time, one day he missed walking. One day, when his counts were the lowest and his stomach was protesting the assault of the beneficial poisons. But always he remembered… keep moving. With a shaky hand, he reached for the two bottles of ensure that were on his meal trays and began arm exercises using those bottles as weights. Keep moving.
That has been his way throughout our journey.
Movement will help. Push past the fatigue and fog and keep moving. Leg lifts in the recliner, exercises with a walker, using household objects to work the arms.
And then congestive heart failure comes to roost and he’s limited. Limited in what he can lift, push, pull, carry. Inclines can’t be traversed. Care to be taken.
The universe has changed the rules and accepting these changes is hard. The ramifications of pushing past is no longer simply a day of rest and recuperation. His heart isn’t cooperating. After overdoing, his blood pressure drops. Less oxygen to the brain leads to confusion, slurred words, frustration, fluctuations in mood. Anyone who didn’t know better, would think he was drunk. Days are needed to recuperate.
It took us a while to put two and two together on this. At first we thought it was the meds as these episodes seemed to happen whenever there was a change in dosage. What really seems to be the case, is that the change in dosage gave Rich a bit of a boost which gave him a false sense of healing. So, he walked. And lifted. And had these episodes of ataxia.
For close to six months, lifting more than he should or exerting himself with exercise that formerly would have done more than send him for a nap, now had him on a different kind of roller coaster… one that set our house into chaos.
The hardest part of this carnival ride was for Rich to accept limitations. Our conversations with our gurus seemed to always include discussions on fatigue. Rich would bring up his disappointment in the backward progress of his energy levels. And what we would experience if he did too much. Like many a four-year-old, he tested his boundaries and not often to a good effect. Our conversations at home were like nagging on my end and whining at his. This isn’t the way we expected our lives to be although, honestly, the man IS still technically a toddler! But how to put a grown man in time-out?
With any disease or injury that has lasting effects, there is a mourning period. No longer is the person who they once were. Physically, mentally, emotionally, there are changes. And the mourning is not just limited to the patient but encompasses all who know and love them. The trick is to not let this mourning dictate the future. Our wise man of the geodesic domes Buckminster Fuller said, “You never change things by fighting the existing reality. To change something, build a new model that makes the existing model obsolete.” It was time for that change. It was time to act for that change. As always, it was for us to change and fit into the existing reality in a way that would work for us.
To that end, Rich and I puzzled the differences over the past year. We looked at his energy camping with Jake in July… hiking in Ireland in September. The decrease in abilities for distance. The walking had stopped. We looked at the episodes of seeming ataxia. We tried to figure out causes…. And solutions. How to make that change we wanted actually to happen?
This month something clicked. One year since the idea of congestive heart failure was brought up, it was like a light switch went off.
When we visited the heart failure guru, we were thrilled by her comments on Rich’s progress; he’s now maximized and optimized on his medications. He is tolerating them well. His kidney function is still off but stable. All what she and we hoped for. And yet, she had concerns. His fatigue. It was time to address it.
First, she suggested we see a sleep specialist and set up an appointment to see if Rich had what is called central apnea. Unlike obstructive apnea, this is a failure of the brain to transmit the proper signals to breathing muscles. It literally forgets to say “breathe!” While this type of sleep apnea is uncommon as compared to obstructive apnea, it is a risk for those with congestive heart failure. The symptoms seem to fit. She sends a request for an appointment to the proper department.
Next up, we discussed a more interventional solution. On the current medications, Rich’s ejection fraction (EF) has improved to where it is now close to the 40% it was and has been following his 2004 chemo. The cut-off for an implanted defibrillator is 35% and we are well past that. Now a normal EF is generally 65%; meaning 65% of the blood in the left ventricle is pushed out with each heartbeat. Below 35%, the heart needs some internal help.
Our heart failure guru feels that Rich may benefit from, not a defibrillator as originally had been discussed, but a pacemaker. That extra boost would help him maintain his energy. Other patients like him have. To see if it would be an effective protocol, we’re advised to have a CPET… a cardio pulmonary exercise test. This, unlike a stress test, would be on a stationary bicycle and would monitor, not just his heart and breathing rates, but the amount of oxygen his body, his muscles, are using and how much CO2 he is producing. Enzymes, mitochondria, heart, valves, lungs… the data that it can gather is stunning. And will answer questions… many more than we’ve had answers to before. And all from a simple bike ride.
And, she suggested, that if we were to go with a pacemaker, if the test indicated it would be helpful, then we should have the coil wiring implanted at the same time as well that would be viable for a defibrillator… in case in ten years or so it may be needed, it would be a simpler procedure just to switch out the box.
Ten years. Ten years. TEN! Instead of the heart transplant she first discussed with us, now we’re talking a quick change of a small box… if necessary. Y’know that stinging feeling you get when tears are imminent but you’re trying to keep it all in. Yeah, that. Suddenly, we’re talking a whole new outlook.
But first, a little reality hits. Rich is buoyed by the doctor’s assessment and, in doing so, goes overboard on activities the next day. By the time I get home, we’re in ataxialand. And we’re in deep. There is a double-edged sword to this; on one side, anything I say he will forget and on the other, anything I say he will forget. If marriage is a series of compromises, then sometimes we all bite our lip and are careful in our words. But to paraphrase the question of that tree in the woods, if a wife yells and the husband forgets it, does it exist? This could be a very cleansing opportunity!
Do we take advantage of this? We do. But the yelling is of truths and frustrations and despite the volume, they are heard. Yelling becomes talking and the talking builds from the truths and the frustrations that were said. And time passes and we keep talking. We revisit activities he has enjoyed in the past and discuss how to make them fit his current reality. We talk about possibilities. We talk about patience. We talk about us. Whether this is the pivotal moment or other factors are at play, acceptance is in the house. It was a long night.
Two weeks have passed without an episode. Rich has become active in the garden. Small tasks that are within his current wheelhouse are being done daily. He is more in tune with when he is reaching the tipping point. He takes those moments to stop and rest. Due to a knee injury he can’t take the CPET testing yet. He also delays his cardio rehab that was scheduled to begin next week. Setbacks but otherwise making progress.
Setbacks. I get home from work after writing these words and again we’re in the land of ataxia. This time we surmise it’s carrying a heavy box from Amazon and some solo food shopping the associated bags that weigh more than they should. BP drops, wonkiness rises. It’s another long night. But it’s just a blip… it doesn’t feel like it but we learn from it and move on. Keep moving.
So as the weather begins to warm and the days are noticeably longer, as his knee begins to heal, walking will happen again. In preparation, we work to schedule ketamine infusions to stem the neuropathy pain that is beginning again. We’re getting ready. The park is waiting.
“How often I found where I should be going only by setting out for somewhere else.” ~ BF


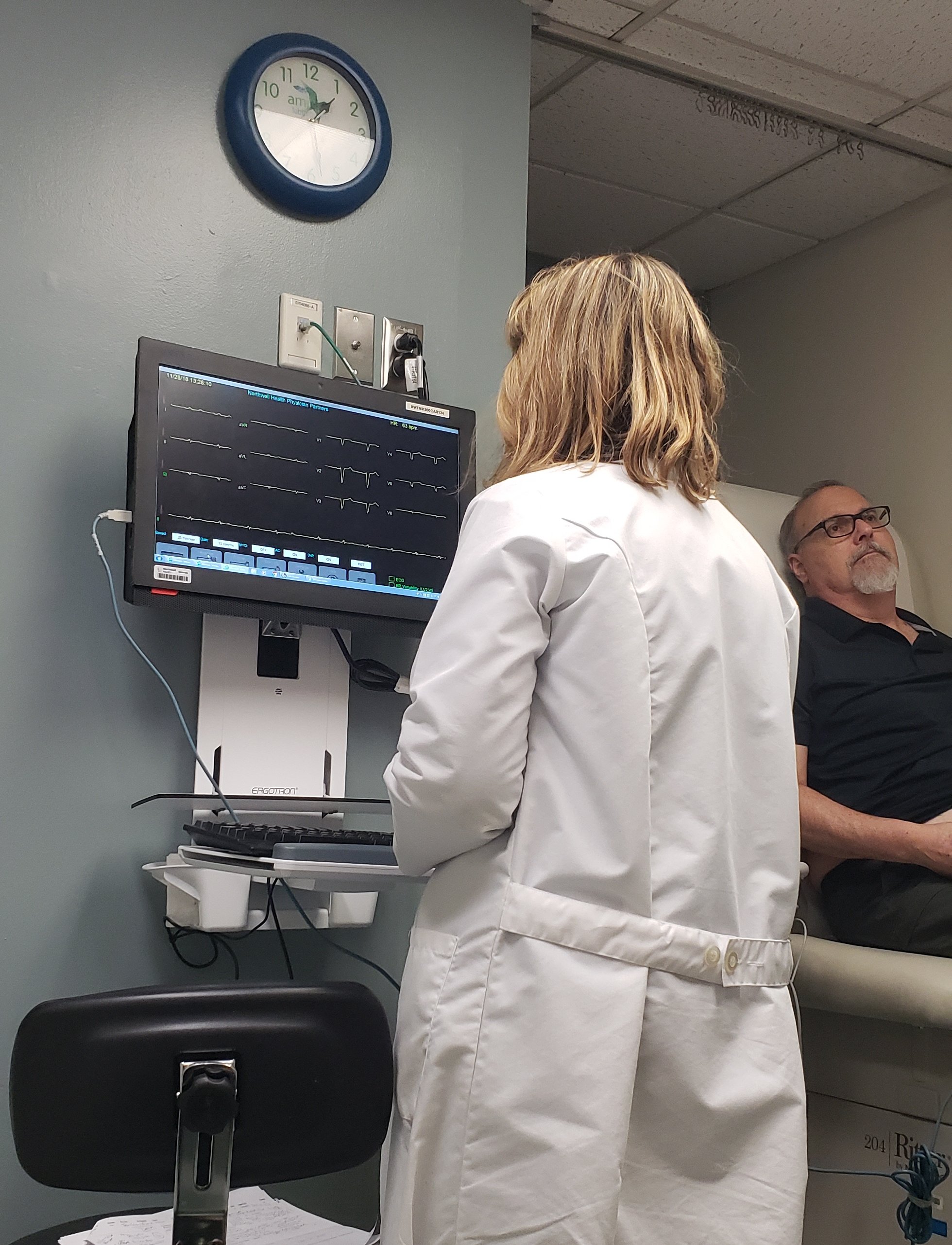





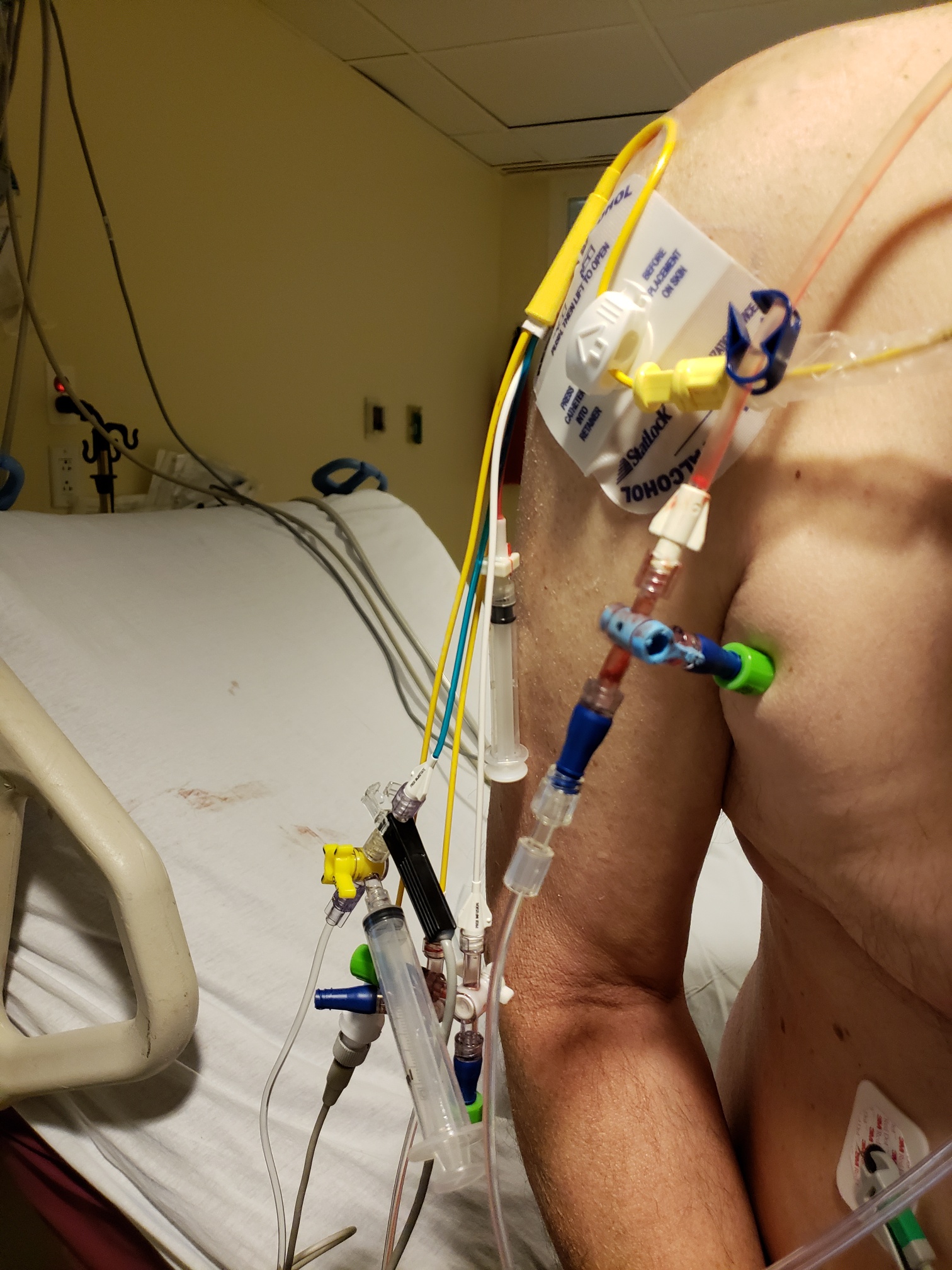


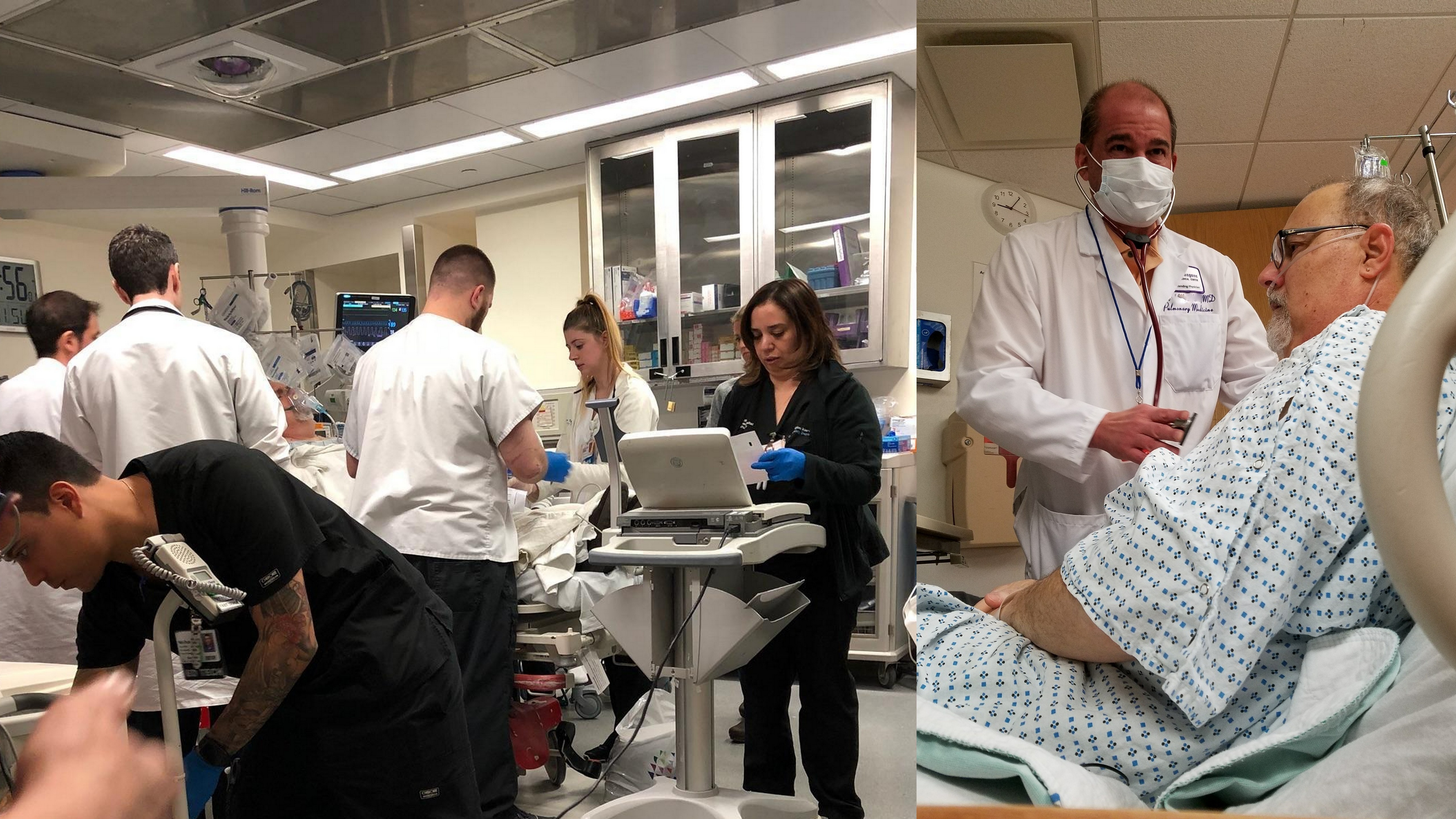
 Weighing our options, we decide to give it a try. Our hope then and now is that it would allow us to wean off the other meds and lower Rich’s dependence on prescriptions for relief. And so, we began. Unlike so many other infusions, Rich is alone in the treatment room; I’m not allowed to stay. The idea is to keep him quiet and still. With possible side effects, all variables are removed. No music, no reading. Low lights, warm blankets and a slew of leads checking his vitals sticky taped to him everywhere. He is under constant monitoring. Over a period of four hours, a small dose of ketamine drips ever so slowly through the IV and into his arm. He dozes.
Weighing our options, we decide to give it a try. Our hope then and now is that it would allow us to wean off the other meds and lower Rich’s dependence on prescriptions for relief. And so, we began. Unlike so many other infusions, Rich is alone in the treatment room; I’m not allowed to stay. The idea is to keep him quiet and still. With possible side effects, all variables are removed. No music, no reading. Low lights, warm blankets and a slew of leads checking his vitals sticky taped to him everywhere. He is under constant monitoring. Over a period of four hours, a small dose of ketamine drips ever so slowly through the IV and into his arm. He dozes. The effects of the drug as well as the relaxant they give him to forestall any hallucinatory dreams gives him rest. He’s released with warnings as if he’s had surgery. In truth, the experience is exactly the same, just without a knife. As we wait for our ride home, Rich realizes that he has no spiking pain and we share a grin. When he gets home, he sleeps.
The effects of the drug as well as the relaxant they give him to forestall any hallucinatory dreams gives him rest. He’s released with warnings as if he’s had surgery. In truth, the experience is exactly the same, just without a knife. As we wait for our ride home, Rich realizes that he has no spiking pain and we share a grin. When he gets home, he sleeps. So for our anniversary in November, shortly after the last infusion, we take our Amtrak train and spend an extended weekend sleeping, eating and roaming in nothing but historic buildings. When the tiredness hits, we only have to look out through the old wavy glass pane of our room where once Martha Washington’s family lived to watch the fife and drum corps make its way down the street. To see groups wandering by lantern light. And when rested, to step out our door and cross the cobbled streets to the nearby tavern for a few small plates and to raise a glass to the musicians performing. As with all our travel, we are renewed.
So for our anniversary in November, shortly after the last infusion, we take our Amtrak train and spend an extended weekend sleeping, eating and roaming in nothing but historic buildings. When the tiredness hits, we only have to look out through the old wavy glass pane of our room where once Martha Washington’s family lived to watch the fife and drum corps make its way down the street. To see groups wandering by lantern light. And when rested, to step out our door and cross the cobbled streets to the nearby tavern for a few small plates and to raise a glass to the musicians performing. As with all our travel, we are renewed.
 As we sit on the swing by our little pond, we watched the butterflies flitting about the garden. A copper-roofed birdhouse swings in the breeze. From under that little roof bits of dried grass, yarn and the flotsam and jetsam that make up a finch’s nest have been pushed out the side. Our occupant has begun re-arranging the furniture to prepare for the next batch of eggs.
As we sit on the swing by our little pond, we watched the butterflies flitting about the garden. A copper-roofed birdhouse swings in the breeze. From under that little roof bits of dried grass, yarn and the flotsam and jetsam that make up a finch’s nest have been pushed out the side. Our occupant has begun re-arranging the furniture to prepare for the next batch of eggs.